Significance of Nucleated Red Blood Cells as a Predictor of Clinical Outcome of Asphyxia in Neonates
DOI:
https://doi.org/10.14740/ijcp1036Keywords:
Nucleated red blood cells, Neonate, AsphyxiaAbstract
Background: Neonatal asphyxia is a leading cause of premature death and a significant concern in Indonesia. An increased number of nucleated red blood cells (NRBCs) at birth reflected hypoxic conditions during late pregnancy and delivery, and functioned as a prognostic biomarker for complications related to asphyxia. NRBCs served as a prognostic biomarker in predicting complications of asphyxia. This study aimed to show that NRBCs levels could predict mortality in neonates with asphyxia.
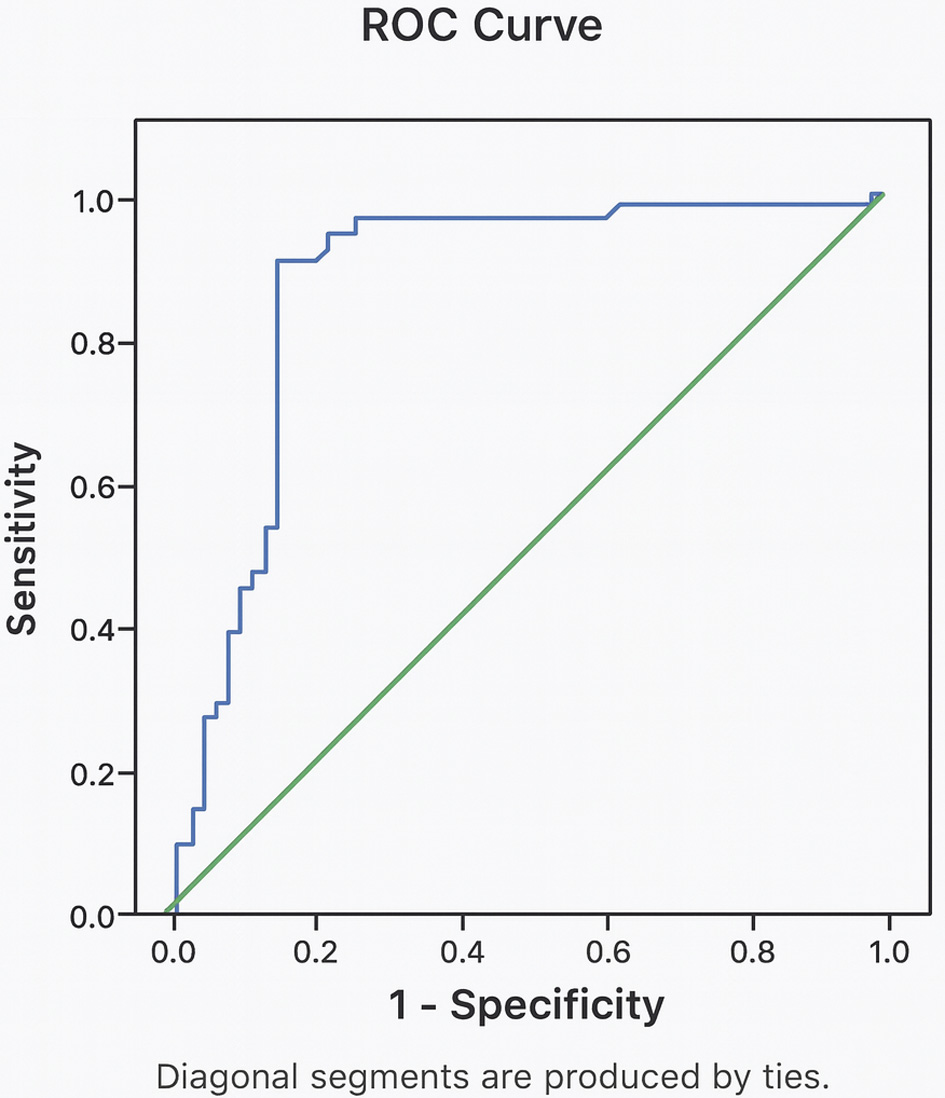
Methods: A total of 108 neonates with asphyxia in the neonatal intensive care unit (NICU) were included in this study. Hematology examinations were carried out on the neonates, and diagnostic testing used the cutoff value of the receiver operating characteristic (ROC) curve. Furthermore, the Chi-square test and logistic regression were carried out to determine the independent relationship between NRBCs levels and mortality in neonatal asphyxia.
Results: A cutoff value of 1.28/µL was used for absolute and relative NRBCs levels, leading to a sensitivity and specificity of 83.67% and 84.75%, respectively. Furthermore, a cutoff value of 10.5% was used for relative NRBCs levels, leading to 81.63% and 81.36% as sensitivity and specificity, respectively. Multivariate analysis showed that absolute NRBCs levels influenced mortality in neonatal asphyxia, with a prevalence ratio of 10.332.
Conclusion: Absolute NRBCs levels could be considered a predictor of mortality in neonatal asphyxia.
Published
Issue
Section
License
Copyright (c) 2026 The authors

This work is licensed under a Creative Commons Attribution 4.0 International License.






